Impact of Low Income Families Not Accessing Care for Disabled Chidlren
- Research article
- Open Access
- Published:
Barriers and facilitators to healthcare access for children with disabilities in low and middle income sub-Saharan African countries: a scoping review
BMC Health Services Enquiry volume twenty, Article number:15 (2020) Cite this article
Abstract
Background
Children with disabilities (CwDs) brand up effectually 150 million of the billion people with disabilities in the earth. The Sub-Saharan African countries accept a large number of CwDs who have limited access to healthcare and rehabilitation care. This, combined with chronic poverty, low education, and inadequately trained healthcare professionals, substantially lowers these children's quality of life. The primary objective of this scoping review was to discover the barriers and facilitators to healthcare access for CwDs in selected low to middle income Sub-Saharan African countries. Every bit African countries significantly vary in socioeconomic status, nosotros simply focused on countries in Sub-Saharan Africa who allocated less than $50/person to healthcare.
Methods
A broad and iterative search strategy using multiple sources and databases including CINAHL, Medline, Global Wellness, and Embase were utilized. Using a comprehensive search strategy, 704 articles were generated. Afterward removal of the duplicates, 466 of them were screened based on the study inclusion and exclusion criteria. After iterative reading and screening of these articles, a terminal 15 articles were included in this review.
Results
This scoping review shows that CwDs in the selected Sub-Saharan African countries face major barriers including stigma and negative attitudes, poverty and insufficient resources, inadequate policy implementations, concrete inaccessibility, lack of transportation, lack of privacy, and inadequately trained healthcare professionals to bargain with disability. Emotional and social back up, including peer back up for CwDs and caregivers, were identified as facilitators for ameliorate access to health services.
Conclusions
There is express access to healthcare services in the low and middle income Sub-Saharan African countries due to poverty, low education, inadequate healthcare systems, and shortage of healthcare professionals. It is evident that in that location are socioeconomic, cultural, and physical related impediments that impact CwDs' and their caregivers' access to the required healthcare services. Policy development, improved physical accessibility, public disability awareness, and parental support are some of the cardinal facilitators to admission healthcare services. The report highlights the importance of revisions to childhood disability and healthcare provisions policy and do as well equally sustainable rehabilitation programs. Further research is required to explore ways to improve feel of accessing health services.
Background
The Un International Children's Emergency Fund (UNICEF) reported that the global rate of child disability is high and at that place are approximately 150 million children with disabilities (CwDs) [1, 2]. The Sub-Saharan Africa is dwelling to a large number of CwDs, many of whom lack access to basic healthcare services [3].
International organizations such as WHO and UNICEF work to address the needs of children in underdeveloped countries and state of war-torn countries [two, four]. WHO declares [1] the back up for people with disabilities as a human rights outcome [2] and describes mainstreaming disability as an of import development result. However, there is a lack of disability sensation, services, and inquiry in almost all of the Sub-Saharan African countries [iv] . UNICEF expresses that CwDs often do not survive their childhood or for those who practice survive, their conditions become worse due to lack of basic principal healthcare service provisions.
Many CwDs and their families exercise not have equal access to healthcare services compared to children without disabilities, practice non undergo treatment or inability-related services, and are overall excluded from everyday life activities [4] . Bones healthcare services are defined every bit the least healthcare needed to maintain sufficient wellness and protection from disease [five] . Access to healthcare services exists when services are available in enough supply and when there is an opportunity to receive healthcare. Barriers to wellness services tin can arise when there are financial, organizational, social, or cultural strains within the community [6]. In many Sub-Saharan African countries, accessing healthcare services and rehabilitation services for CwDs is limited to urban areas, if available at all [3]. When children miss out on essential treatment for bones illnesses such as fever and diarrhea or miss vaccinations, these treatable illnesses ofttimes evolve into lifelong disabilities [2]. Childhood disability in the Sub-Saharan Africa is closely linked to poverty [iii]. When impoverished children experience disability, it is often due to inadequate healthcare services for pregnant mothers and basic healthcare services for immature children [5]. Disability persists and is continuously affected by socioeconomic, political, and cultural situations of a given social club [iii].
There are currently no scoping reviews on the barriers and facilitators affecting healthcare admission for CwDs in the low and eye Sub-Saharan African countries. Therefore, it is important to explore and analyze the existing literature and compile the information in one source for easy access and to develop the next steps for intervention.
Methods
The outline for this review followed the five-phase framework described by Arksey and O'Malley [7]: 1) identifying the enquiry question, 2) identifying relevant studies, 3) study selection, iv) charting the data, and 5) accumulating, summarizing and reporting the results. This newspaper aimed to respond the following research question: "What are the facilitators and barriers to healthcare access for CwDs in selected low and middle Sub-Saharan African countries?". For the purpose of this paper, access to health intendance was defined as receiving appropriate health care resource for the purpose of maintaining or improving health condition [half-dozen]. The term "children with disabilities" refers to children upward to the historic period of 18 who have "long-term physical, mental, intellectual, or sensory impairments which in interaction with various barriers may hinder their full and effective participation in club on an equal basis with others" [8, 9].
Data sources and search
Multiple electronic databases including CINAHL, Medline, Global Wellness, and Embase were used to search for relevant studies betwixt March–July 2017. Manual search was completed using Google Scholar and Queen's Academy Library search engines. Search terms included: "children with disabilities", "barriers to healthcare access", "African children healthcare admission", "facilitators to healthcare access", and "barriers and facilitators to healthcare admission". The selected manufactures were combined into EndNote Basic and duplications were deleted.
Study selection and screening
The search resulted in 704 records. Articles were screened based on their title and abstracts for eligibility and imported into EndNote Basic to remove duplicates. Through independently screening by the reviewers, the remaining studies were then examined further by reviewing their abstracts and removing articles that did not satisfy the inclusion criteria. The remaining papers were so screened for a concluding time through a total-text revision and non-relevant papers were excluded. In that location was no brake on publication date due to express research on the topic. Finally 15 peer-reviewed articles were included in this scoping review.
Articles were included if they discussed barriers or facilitators to healthcare admission for children under the age of 18 in selected low and middle Sub-Saharan African countries. Every bit the African countries significantly vary in terms of their socioeconomic condition, this review but focused on countries in Sub-Saharan Africa who allocated less than $fifty to healthcare per person. This reference signal was used to focus on the countries that were most in need of health resources. This provides useful information about whether the government spends enough of its own resource on health in lodge to provide universal coverage of essential healthcare services, particularly for vulnerable groups such equally children.
Data charting and abstraction
A PRISMA nautical chart and a standardized information extraction course were used. A two-pace charting process was completed using Excel. The beginning step included creating a table and extracting the following information from reading the abstracts of the identified articles: authors/researchers of the article, publication year, report objectives, whether the article was nigh Africa, included children 0–18 years of age, included children with disability, and collected data on access to healthcare service. The next pace of the charting process included extracting the post-obit data from the remaining papers past reading the full articles: authors/researchers of the article, publication date, objectives of the paper, inclusion criteria, historic period and gender of the children, sample size, historic period, income and education of parents, gender of the children, children's pedagogy, type of inability, city, country, and setting of the study, study method, event of the paper, results, facilitators and barriers to healthcare services.
Data analysis
The next footstep of the process included an iterative independent article screening, reading, and theme coding. Abiding discussions on the procedures and emerging problems took place until the researchers agreed and major themes were formed. A card system method [10] was used to come up upwardly with overarching themes and categories across all reviewed articles and synthesized results from reviewed studies. Finally, the major themes that emerged from the data regarding facilitators and barriers to healthcare access to CwDs in Sub-Saharan African countries were identified and discussed.
Results
Study screening results
A full of 466 articles were imported to EndNote, including articles that were identified through manual searches. After excluding articles by examining the title, 314 article abstracts were screened and 27 articles remained for full-text examination. After concluding evaluation, 12 more articles were excluded. 9 qualitative studies, five mixed design studies, and one quantitative study met all inclusion criteria and were used in the scoping review for a total of 15 articles. Come across Fig. i for total commodity screening process.
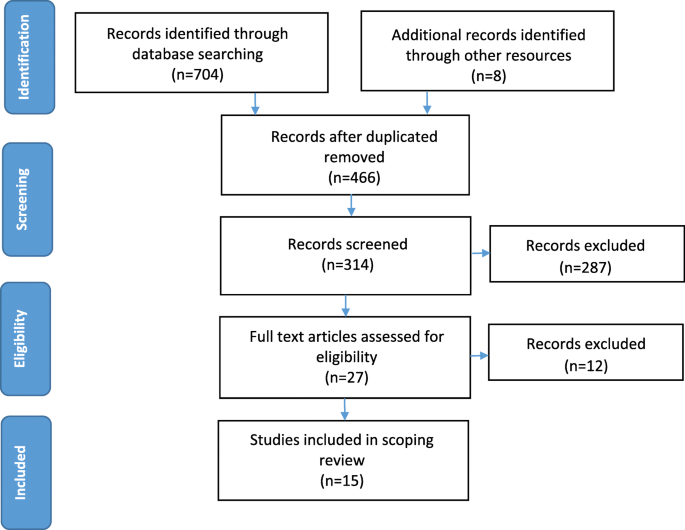
PRISMA period diagram for the scoping review process
Although in that location were 29 countries in Africa that allocated less than $fifty per person to healthcare, papers included in this report were from only 9 Sub-Saharan countries. Of the 15 articles discussed in this review, 4 papers reported on Ethiopia [xi,12,13], two on Republic of zimbabwe [14, fifteen], two on Malawi [16, 17], two on Cote d'Ivoire [eighteen, 19], one on Rwanda and Uganda [20], ane on Uganda [21], one on Republic of kenya [22], one on Republic of zambia [23] and 1 on Nigeria [24] (Table 1 in Appendix).
After extraction of data and comparison and contrasting the results, several themes emerged regarding barriers and facilitators to wellness care access for CwDs in low and heart Sub-Saharan African countries (see Additional file 1 for more details).
Trends in quantitative and qualitative studies
All 15 articles identified barriers to accessing healthcare services for CwDs in selected Sub-Saharan African countries. 14 studies utilized qualitative methods, including mixed methods, and relied on interviews or questionnaires to identify specific barriers. 13 of those 14 articles determined these barriers through interviews and group sessions with the CwDs' caregivers (parents, or any other person who was the main person to take care of the child) or service providers and simply one study interviewed the children themselves [xx].
Theme 1: Attitudes, beliefs and awareness of disability
Stigma
Stigma, including experienced stigma and fear of stigmatization, was a reported barrier in 5 papers. High levels of stigma were reported by many families of children with disabilities, preventing them from allowing their children to access wellness care and proper medical treatment [11, 12, xv, 23] . Caregivers in Federal democratic republic of ethiopia, Republic of zimbabwe, and Zambia expressed concerns virtually being treated poorly by others and how this caused them to decide to hide their child's status instead of seeking handling [11, 12, 15, 23]. A health extension worker in Ethiopia noted that caregivers were ofttimes worried about beingness treated differently, feeling ashamed or embarrassed almost their child'south status, and made efforts to keep their child'south condition a secret [11]. Families were worried that if others knew that their child had a inability, they might never go married due to stigma [12].
Personal and community attitudes
Negative attitudes towards CwDs can affect access to healthcare services and facilities. Negative attitudes both from caregivers and from healthcare professionals hinder accessing healthcare services [11, 17, 20, 21] . For instance, a study showed that negative attitudes well-nigh disability in Ethiopians resulted in lack of support from the community and the children'due south families' which decreased the motivation of health extension workers [11]. Another example of the negative impact of mental attitude on health admission is seen in Malawi where caregivers believed "zilch can be washed" for their kid and therefore did not seek medical treatment [17].
Personal attitudes and beliefs of the healthcare staff in Uganda and Rwanda afflicted the youths' access to healthcare services [20]. One participant in Uganda reported a case where a nurse would not provide HIV related services such as blood tests to a girl with a physical disability due to misconceptions that youth with physical disabilities were non sexually active [20]. Furthermore, caregivers reported that they were sometimes rejected by healthcare workers and their children did non receive treatment considering some healthcare providers believed that these children could not be treated [xiii, xv, 23] . A written report past Bannick and Stroeken [21] found that parents of CwDs were often discouraged from seeking healthcare services for their child as information technology was perceived as a waste of coin. Parents in this report were advised past others in the community to leave their child to die or that their child was "already dead [21].
Despite the fact that there were challenges and barriers that prevented accessing healthcare by CwDs, a positive mental attitude amid family and community members tin can encourage caregivers to seek treatment for their children. Family members were more probable to encourage parents to seek treatment for their children when they noticed an improvement in the kid's health as this gave them a sense of hope. Bannink et al. (2015) and Nota et al. (2015) found that when a kid showed visible and observable health improvements, such as surgery recovery or significant rehabilitation progress, the community's attitudes changed and became more than positive and supportive [fifteen, 21].
To annul the mental attitude of caregivers, the literature suggested making treatment sessions more attractive to the caregivers. Having longer therapy sessions was reported to be a facilitator for attention therapy sessions in Republic of zimbabwe [15]. Nota et al. (2015) establish that caregivers were less probable to miss their child's therapy sessions if they were group sessions as opposed to individual sessions. The authors suggested that the group setting immune caregivers to share their experiences with each other and with the healthcare workers equally well as compare their child'southward progress to other children. These interactions would also create meaningful relationships between the caregivers and the healthcare workers, allowing for improve treatment outcomes for the children and therefore encouraging parents to proceed with the treatment [15].
Lack of sensation
Disability awareness refers to factors that acquaintance with being educated on and understanding inability. Attitudes were considered distinct from awareness in that awareness is related to education while attitudes were related to personal or cultural beliefs. A well-informed customs almost inability and how to identify children with disabilities (i.e. a college awareness), would provide an encouraging context for children accessing services.
The literature showed that a lack of inability awareness acted equally a substantial barrier in the community to seeking treatment. Many caregivers in Ethiopia lacked awareness of their CwDs. They did not recognize their children as people with disabilities or they did not admit their children's needs of seeking medical attention [12, 13]. Some caregivers believed their child was disabled due to head injury, birth complications, epilepsy, or religious causes. As a result, a large number of caregivers sought out traditional places for care rather than medical attention [xiii]. Shibre et al. (2001) found that many caregivers only relied on prayer to address problems of their child's disability [12].
Lack of awareness affected health care professionals likewise. For example, health extension workers in Ethiopia expressed the need for in-service training to identify causes, prevention, and treatment for children experiencing mental health and developmental disorders [11]. They described having poor knowledge on kid developmental disorders and reported that this lack of skills and knowledge lowered their conviction when working with the children and their families [eleven].
Co-ordinate to Tekola et al. (2016), sensation-raising activities of ii autism centers in Ethiopia, the Joy and the Nehemiah, helped to educate and inform the public and the healthcare staff nigh the illness, conducting diagnoses and decreasing stigma, thereby increasing access to healthcare services [25]. However, the centers were express to children with autism spectrum disorder and located in the capital letter metropolis of Ethiopia [13]. Bannink et al. (2015) also stressed the importance of making the community more aware and informed about childhood disability. Being more informed virtually causes and etiology of the disease or disability helped to change the community's beliefs and perceptions and proceeds back up for children with disabilities and thereby reducing stigma [21]. There was testify that educating caregivers about the child's condition tin can also positively impact access to health services. CwDs were often neglected by caregivers and not taken to healthcare facilities and rehabilitation appointments [17]. Paget et al. (2015) institute that caregivers were less probable to neglect their children when they were educated about their condition [17]. This awareness allowed parents to exist more informed, agreement, and accepting, which increased their likelihood of seeking and continuing treatment for their children [17, 21]. However, it is of import to note that visible health improvements in children were a stronger facilitator, compared to awareness, in changing attitudes. Bannink et al. (2015) reported that even when family members were informed most the child's inability and rehabilitation handling, their attitudes did not change until they saw noticeable improvements in the child's health condition [21].
Cultural beliefs
Cultural beliefs also prevented CwDs from accessing wellness care services [thirteen, 19, 21, 23]. Studies reported on the belief amongst African communities that having a kid with a disability was a punishment from God or the child was possessed by the devil [13, xix]. In Ethiopia and Zambia some people believed that disability was a source of witchcraft, curses, and bad luck [13, 19, 21, 23]. These beliefs prevented parents and caregivers from seeking health care handling for their kid. In Uganda, mothers of children with spina bifida and hydrocephalus were feared in their communities as they were seen as having given nascence to a demon [21]. The mothers were discouraged from taking their child to the hospital and from engaging in vital practices such as breastfeeding. Instead, parents were encouraged to accept their children to witchdoctors to remove the curse [21]. Bannick et al. (2015) too described a common practice in Northern Uganda where mothers would carry their infants on their backs, become to the river, and untie the wrap carrying the child. The death of the kid would and so be reported every bit an accidental drowning [21]. Similarly, in Cote d'Ivoire, CwDs were often isolated and in some cases killed out of fear of harming others [xix]. Paget et al. (2016) found that CwDs were at risk of parental abuse and fail [17]. Healthcare workers in the study indicated that neglected children were oft left alone and locked up, non cared for, not fed, and not taken to healthcare services [17]. Some healthcare professionals in Cote d'Ivoire and Republic of uganda were reluctant about the idea of providing CwDs with healthcare services due to the cultural beliefs surrounding the etiology of disabilities [19, 21]. In Uganda, some healthcare workers refused to treat children with spina bifida and hydrocephalus as they preferred not to deal with what they referred to equally "special cases" [16, 21].
Theme 2: Accessibility of services and systems
Availability of health services, clinical pathways, and qualified healthcare staff
Available enquiry showed that CwDs in Zambia, Malawi, and Kenya take limited admission to healthcare services including community and hospital services in populated areas [16, 22, 23]. Therefore, caregivers would take their children to exist treated by traditional healers instead of seeking medical attention [23].
Lack of qualified healthcare professionals had a pregnant impact on the quality of the healthcare services, which can deter caregivers from using those services. In Ethiopia, for instance, a big number of children with autism and intellectual inability remained without official and validated diagnoses due to lack of awareness, teaching, and preparation for healthcare professionals and staff [xiii]. Tekola et al. (2016) and Tilahun et al. (2016) indicated that there was inadequate medical handling for children with autism and intellectual disabilities in Ethiopia where the population is over 100 million, with only ii treatment centers located in the capital city, Addis Ababa [13] . In 2016, in that location were just ii child psychiatrists in Federal democratic republic of ethiopia and no psychologists were trained in child mental health [xiii]. Yousafzai et al. (2005) institute that communication was a barrier for deaf teens in Republic of uganda when trying to access HIV healthcare service [20]considering most healthcare workers did not know sign linguistic communication. This lack of training for the staff prevented teens with disabilities from beingness able to communicate with healthcare staff and therefore from accessing services [20]. In Malawi and Uganda, similar findings were observed in which healthcare workers lacked awareness of services and did not have access to standardized cess procedures for child mental health [17, 21].
Healthcare workers were oft unclear almost referral pathways and displayed poor communication skills. Therefore, when healthcare was needed, it was not adequately provided to these children [17, 20, 21]. It was unclear within the articles what these services and standardized assessment procedures should be. Furthermore, in Malawi, caregivers expressed their concern about not finding services for their children's specific inability, such as an ear clinic for hearing disabilities and physiotherapy for physical related disabilities. They also described not having wellness facilities in the surface area they lived in, thereby making it difficult to even find a service [sixteen]. In Republic of kenya, although physiotherapy was present within health-based rehabilitative services, adults with disabilities were prioritized and inadequate service was provided to children experiencing disability [22]. In Republic of zambia, due to lack of related policies and processes, information technology was not possible to properly plan to place, administer care and follow up with children experiencing disability. Health intendance workers as well blamed heavy workloads, limited staffing, and inadequate training for inadequate care [23]. Other researchers institute that there were very little rehabilitative staff and lack of health care workers, making it extremely challenging to provide access to healthcare services to all CwDs [11, 17, 22, 23]. In Zimbabwe, Nota et al. (2015) also found that the availability of the rehabilitation staff was a facilitator for caregivers to access the rehabilitation services. Caregivers were more motivated to admission healthcare services if the rehabilitation workers were available to provide required services every time the children visited [15].
The literature suggests three means to change the procedure of care to improve health access. First, allowing caregivers and CwDs to be active participants in the process of intendance equally opposed to passive recipients. When parents and children had a say in the handling process, they were more likely to exist motivated to access those services [15, 21]. The second way to improve health access is by using an interdisciplinary approach throughout the process of care. When professionals from different disciplines collaborated, they were more likely to provide the best possible care for the child and this in plough motivates caregivers to bring their children to those healthcare services [21]. Finally, using a holistic approach in which all rehabilitation services are offered in one location, such as in the same hospital, can help improve health admission. Caregivers in Zimbabwe noted that this was a motivator for them to admission those services [15].
Magnussen and Ingstad (2011) constitute that 1 of the reasons caregivers of CwDs did not access [15] healthcare services in Zambia was due to a poor reputation of the healthcare facility [23]. As a result in some cases, although the facility existed, information technology might not be used by families of CwD because of poor reputation. In tightly knit communities, the opinions of the community impacted the caregivers' opinions and how much they used those facilities. The report reported that this barrier was overcome through the use of neighborhood health committees and customs volunteers in Zambia who helped identifying CwDs in the community. According to Magnussen and Ingstad (2011), access to healthcare facilities in Zambia was improved by enhancing the reputation of those health centers. Positive experiences shared with others changes the customs's attitudes about the facility and motivates others to access those services [23].
Availability of resources, equipment, and funds
Research showed that limited funding and resources negatively impacted intendance for CwDs. Many healthcare facilities were underfunded and this in turn affected the access by CwDs [11, 16, xviii, 22]. For example, in Kenya, staff described that as a issue of express funding, CwDs had limited access to effective services because of low staffing, depression quality resource, and old equipment [22]. In Malawi, Paget et al. (2006) identified that healthcare workers tried their best to provide treatment and service to CwDs and their caregivers, however, they faced lack of space to provide handling, lack of equipment to assess and transport children, and limited access to medicine to provide to children who were medically unstable [17]. Devendra et al. (2013) reported that in Republic of malaŵi, only 5% of 98 CwDs who attended rehabilitative services received rehabilitative equipment. Having enough funding was a facilitator for ameliorate access to services. Most caregivers believed that if their children had admission to equipment such equally hearing aids, wheelchairs, bicycles, crutches, walking aids, and glasses, it would help with their handling and amend their access to service [xvi].
Theme 3: Physical surroundings
Transportation and weather conditions
Travelling with a kid with a disability tin can be quite difficult for caregivers, especially if the child used heavy assistive devices such every bit a wheelchair or if the family lived in rural areas far from the health facility. This can hinder families from accessing those services or from taking their child with them to medical appointments [xiv, fifteen, 23].
Parents expressed difficulty travelling with their disabled children as they would have to acquit them on their backs [14, xv, 23]. In Zambia, healthcare services were scattered in rural areas and therefore people had to walk long distances to admission services [23]. It was especially hard to get around during and afterward poor atmospheric condition atmospheric condition such as heavy rainfall. Roads were oft blocked and became inaccessible due to the heavy rainfalls and floods. Therefore, this prevented people from accessing and using healthcare services in those areas [23]. Health facilities in Malawi [16, 17], Ethiopia [13], Uganda and Rwanda [20], and Republic of kenya [22] were also far apart and caregivers of CwDs, especially those living in rural areas, struggled to admission them due to travel distance, difficulty travelling with their children, or high transportation fees. In Uganda and Rwanda, many health facilities were far abroad and youth with physical disabilities struggled to access them equally they couldn't walk the distance [xx]. In Federal democratic republic of ethiopia, a child can only receive a formal autism diagnosis from government or private mental health clinics in Addis Ababa. Notwithstanding, the government clinics could only exist accessed later a referral and families living in remote areas often did non have access to a referral process. Those who managed to access referrals were often unable to travel the long distance to these clinics [13]. Finkenflugel and Van Maanen (1996) found that this bulwark was overcome in Zimbabwe through the use of community-based rehabilitation (CBR). Since CBR took place in the child'south dwelling house, the service was provided more effectively than using traditional healthcare facilities [14].
Physical inaccessibility
Physical barriers also tin hinder CwDs accessing healthcare. Yousafzai et al. (2005) institute that teens with physical disabilities in Republic of uganda were not able to nourish community healthcare meetings regarding HIV because the locations were physically difficult to access. In Rwanda, it was reported that children with concrete disabilities were unable to visit wellness facilities because they were impossible to access [xx]. These authors, however, did not written report what made the environment physically inaccessible.
Physical inaccessibility was not just nigh getting in and about a facility, rather, was also about using the available resource. Research showed that resources such as data leaflets, flyers, and impress materials was not accessible past CwDs and this limited their access to services as they were non able to reach the data being communicated [xx]. For instance, information almost healthcare services conveyed over the radio was not attainable by deafened teens in Uganda and Rwanda. Similarly, posters were not accessible past children with visual impairments in Republic of uganda and Rwanda. These communication barriers prevent CwDs from knowing virtually and therefore accessing those healthcare services [20]. Providing information in alternative format was suggested every bit i of the solutions.
Theme 4: Social factors
Poverty
Poverty was reported to be a recurring barrier for CwDs and their families. Caring for a CwDs can be expensive as they may require special food, assistive devices, and transportation fees for medical appointments [fifteen]. Tilahun and Hanlon surveyed caregivers in Ethiopia and establish that i of the most unmet needs was lack of financial support. Without fiscal back up from family unit, the regime, or other organizations, information technology was difficult for CwDs to access healthcare services [13]. Express funds tin can forbid caregivers from paying for private services and transportation fees [15, 16, 20, 22, 23], healthcare fees/bills [21, 22], assistive devices [21] and more. Families living in poverty had to ration and prioritize their spending and they often could not afford expenses to healthcare of their CwDs [17, 23]. Health extension workers in Ethiopia indicated that families experienced challenges such every bit transportation and treatment costs that limited their admission to proper handling [11]. Nota et al. (2015) constitute that caregivers in Zimbabwe experience financial difficulties that prevented them from accessing healthcare and fabricated them more likely to miss their kid'southward scheduled therapy appointments [fifteen].
Attention wellness related visits can threaten the family breadwinner'south employment. In Zimbabwe and Zambia, caregivers plant it difficult to access healthcare services because it was difficult to ask for time off of work, especially to attend several therapy sessions [15, 23]. They further described that there were long wait times at the children's rehabilitation clinics that impacted the parents' job [15]. This was specially difficult for families experiencing poverty and single caregivers [23].
Lack of financial support from the family was another fiscal aspect to consider. Caregivers described that fathers would often carelessness the family of the disabled child and would not back up the child financially [21]. This made it hard for the child to receive medical attention as it caused financial and social strain on the female parent, who would become the sole provider for the child.
Financial support from the government or organizations was a strong facilitator to accessing healthcare services, especially for economically disadvantaged families [15]. A study conducted in Zimbabwe found that caregivers of children with congenital diseases were more than motivated to take their children to therapy sessions if incentives, such every bit toys, transportation coin, nutrient, assistive devices, and clothes, were given at the rehabilitation department [15]. These incentives allowed the child to be more than functionally independent and decreased the financial brunt on the caregiver.
Lack of privacy
In Republic of uganda and Rwanda, lack of privacy was a major business organisation for adolescents with disability to admission health care especially for those with hearing impairments [20]. Adolescents explained that they often needed a helper to assist them to medical appointments and this breach of privacy oft prevented them from going to their appointments. They also described that although confidentiality was acknowledged by the healthcare staff, they were concerned that the third person (i.due east. the assistant) would gossip [20].
Peer support
Parents and caregivers were more likely to admission healthcare services and go on treatment for their children if they received emotional and psychosocial support from friends and family unit members [13, 15, 23]. In Zimbabwe, caregivers reported existence motivated to attend therapy sessions by receiving emotional support from other caregivers of CwDs [xv]. Research as well showed support of peers was important to both CwDs and their caregivers. Children had better access to health care services when other family members provided social support [23]. In addition, peer support was a mutual coping strategy for caregivers of CwDs [13].
The utilize of back up groups for caregivers was a facilitator for accessing healthcare services [17, 21]. In Republic of malaŵi, health care workers noted that support groups helped inform and empower caregivers of CwDs. The groups provided parents with emotional and psychosocial support that helped them cope with their child's illness [17]. The health intendance workers besides suggested that inviting family members to these peer support groups may assist to enhance sensation and decrease stigma [17]. Similarly in Uganda, parent back up groups allowed parents to encourage and empower each other to fight the stigma in their communities [21]. Parents as well noted that the support they received from the parent support groups helped them feel less worried nigh their child's condition [21].
Give-and-take
The present review identified 15 peer-reviewed articles that discussed healthcare access for CwDs in Sub-Saharan African countries that allocated less than $fifty per person on healthcare spending. This review is the first scoping review to examine barriers and facilitators to healthcare admission for CwDs in Africa. Having identified these factors, recommendations can then be put forth for developing intervention plans.
The findings of this review suggest that there are commonly reoccurring factors preventing caregivers from accessing healthcare services for their children in Sub-Saharan African countries. These factors were identified in different communities across the selected countries where the reviewed studies were conducted. Facilitating factors to healthcare access were non as axiomatic in the literature equally barriers, which may be due to limited scientific inquiry and publications on this topic and the lack of intervention in these countries.
Poverty was the well-nigh reported barrier preventing CwDs and their caregivers from accessing healthcare services; it was discussed in 6 papers in 5 unlike countries. In Nigeria, for instance, poverty was the most influential factor affecting healthcare service use for children and their mothers [26] . Most healthcare services were not costless, even in missionary hospitals where information technology was complimentary in the past [27]. The conditions of the hospitals were poor as they were usually unclean and crowded and lacked funding and medical staff, with much of the work existence carried out by overworked nurses. When families can barely beget to live, taking their CwDs to therapy may not be a priority for them. Shillingford (2010) reported that people in Republic of uganda could not even afford to buy food [27]. In Uganda, individuals were not admitted to the hospital unless they were accompanied by a relative who volition regularly take care of them by feeding and bathing them during their stay at the hospital. Therefore, individuals who were unable to beget to take care of themselves may exist reluctant to take their family members to the hospital. Nota and Chikwaha suggested that providing incentives such as toys, transportation coin, and inability aids may encourage caregivers to bring their CwDs to health facilities [15].
It is evident that religious and supernatural behavior regarding the etiology and treatment of disabilities can affect service admission and delivery. This was perhaps ane of the most powerful barriers to healthcare admission in Africa. Near papers in this study identified cultural beliefs regarding the causes of disability, such as witchcraft, religious penalisation, and possession of evil forces [11, xiii, 17, xix,20,21,22,23,24]. These beliefs were reported in 8 different countries. Although not all papers identified a direct link betwixt these beliefs and accessing healthcare services, there was a clear association between the two. If a family believed their child'due south condition was of supernatural cause, they may never seek medical treatment, no affair how adequate the healthcare staff were. Many families property these cultural beliefs looked for traditional rather than medical handling, such as through prayer or cultural rituals. Aldersey (2014) noted that families in Kinshasa, Congo who viewed the causation of intellectual and developmental disabilities as biomedical were more probable to seek medical treatment for their children [28]. Families who believed in supernatural causes of their kid's disability oftentimes sought out traditional healers or did not seek treatment at all. These behavior also heavily contributed to stigma and this therefore could prevent families from beingness open almost their children'due south weather and from seeking handling. In the literature, stigma was repeatedly found to force families to hide their children, conceal their children's condition, and forbid them from leaving their homes to access a healthcare service or needed handling. Aldersey (2014) found that families of children with developmental disabilities in Kinshasa hid their children at dwelling house and out of sight in guild to forestall others from thinking the disability was a penalization to the family for participating in supernatural practices [28].
In addition to the discussed barriers, other factors can also affect access to healthcare services. A study on healthcare access for typically developing Nigerian children establish that family size had a direct consequence on children's omnipresence to a health clinic, with higher attendance for smaller families [29]. The age of the mother likewise affected attendance. Younger mothers were more likely to take their children to a dispensary for care than older mothers. More educated parents were too more likely to have their children to clinics for immunization than illiterate parents. Perception of disease severity also affected whether or not mothers took their children to health clinics. Mothers were more likely to take their children to wellness clinics for fevers than for peel conditions. Although these findings were for typically developing children in Nigeria, these factors may also affect CwDs and therefore farther studies are needed.
Many papers also highlighted the importance of coping strategies for caregivers and families of children with disabilities. Many caregivers in Malawi and Ethiopia drew on sociocultural and spiritual coping strategies to assistance them obtain hope and meaning [13, 17]. Rehabilitation staff can accept a significant role in supporting families to cope with needs of intendance of a child with disability past beingness mindful of and understanding their patients' social and cultural environment and incorporate this into the goal-setting procedure [30].
Strengths and limitations
A comprehensive literature search was conducted from multiple sources and databases including grey literature for the inclusion of all types of studies from low and middle Sub-Saharan African countries. Even so, in that location were some limitations in this research written report. There was express admission to some articles because they were not available online. Similarly, some authors did not publish their enquiry or only published the abstract, which minimized the overall content of the scoping review. Research on healthcare access for CwDs in Sub-Saharan Africa is already deficient. Only articles published in English were included. Thus, this may have express findings of the study. Due to the express enquiry, articles were not excluded by publication date and therefore the articles in this review ranged from 1996 to 2017. For this reason, another limitation might exist outdated data. However, the themes found in the older articles were also seen in more recent papers.
Implications for babyhood disability policy and practice
It is evident that there is a lack of scientific information about CwDs and their admission to healthcare services in the Sub-Saharan African countries. This may be due to the lack of childhood disability research and interventions. In that location is also low attention about CwDs from the authorities that affects the provisions of healthcare services for CwDs. The Earth Wellness Organization (WHO) as well recommended developing ways to address funding barriers for rehabilitation and healthcare services [4]. Equally this study shows differences in barriers and facilitators, it can indicate future steps or recommendations to inform disability sensation and policy along with intervention strategies on babyhood inability and healthcare provisions. Moreover, the study findings would permit development of sustainable programs such as CBR interventions, which are needed in low and middle Sub-Saharan Africa countries, to remove barriers and increase facilitators to healthcare access for CwDs.
Decision
Attitudinal problems, poverty, inadequately trained healthcare professionals, and concrete inaccessibility are oftentimes reported as major barriers to healthcare access for CwDs in the low and eye income Sub-Saharan African counties. Whereas, efforts for policy development and improving physical accessibility, public disability awareness, and professional and parental support are primal facilitators. Healthcare professionals working with CwDs should be aware of these barriers and facilitators in order to develop effective assessments and intervention plans. To include these children in the healthcare process, in that location needs to exist a greater presence of healthcare professionals, resources, and modifications to healthcare systems. Farther research on pediatric health and childhood disability is needed for enhancing show-based exercise in the Sub-Saharan Africa. More research is needed to further examine access to healthcare for CwDs in the depression and eye Sub-Saharan Africa from the broad perspective of stakeholders including children themselves, parents or caregivers, and healthcare professionals. Thus, future research should investigate recommendations for enhancing access to healthcare services for CwDs in these countries so that action plans and interventions can be designed and put in identify.
Availability of information and materials
Not applicable.
Abbreviations
- CwDs:
-
Children with Disabilities
- UNICEF:
-
The United Nations International Children'due south Emergency Fund
- WHO:
-
World Wellness Organization
References
-
Cameron DL, Nixon S, Parnes P, Pidsadny Grand. Children with disabilities in low-income countries. Paediatr Child Wellness. 2005;10(5):269–72.
-
UNICEF. Promoting the rights of children with disabilities; 2007. [Available from: https://www.unicef-irc.org/publications/474-promoting-the-rights-of-children-with-disabilities.html
-
African Child Policy Forum. The African report on children with disabilities : promising starts and persisting challenges; 2014.
-
World Wellness Organization. World report on inability 2011. Geneva: World Health System; 2011.
-
Mosby's pocket dictionary of medicine, nursing & wellness professions. 6th ed. St. Louis: Elsevier; 2010.
-
Gulliford Chiliad, Figueroa-Munoz J, Morgan M, Hughes D, Gibson B, Beech R, et al. What does' access to health care'mean? J Health Serv Res Policy. 2002;seven(3):186–8.
-
Arksey H, O'Malley Fifty. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(i):nineteen–32.
-
United nations. Convention on the rights of persons with disabilities. New York and Geneva: UNITED NATIONS PUBLICATION; 2008.
-
Groce NE, Deluca Yard, Cole E, Berman-Bieler R, Mitra Thou, Farkas A, et al. Children and young people with disabilities: fact sail; 2013.
-
Goodman MB, Santos GJJCCAIJ. Card sort technique as a qualitative substitute for quantitative exploratory factor assay; 2006.
-
Miftah R, Tilahun W, Fantahun A, Adulkadir S, Gebrekirstos G. Knowledge and factors associated with pain management for hospitalized children among nurses working in public hospitals in Mekelle Urban center, North Ethiopia: cantankerous exclusive study. BMC Res Notes. 2017;10(1):122.
-
Shibre T, Negash A, Kullgren G, Kebede D, Alem A, Fekadu A, et al. Perception of stigma amidst family members of individuals with schizophrenia and major affective disorders in rural Ethiopia. Soc Psychiatry Psychiatr Epidemiol. 2001;36(six):299–303.
-
Tilahun D, Hanlon C, Fekadu A, Tekola B, Baheretibeb Y, Hoekstra RA. Stigma, explanatory models and unmet needs of caregivers of children with developmental disorders in a low-income African state: a cross-exclusive facility-based survey. BMC Health Serv Res. 2016;16(1):152.
-
Finkenflügel HJM, Maanen VV, Schut W, Vermeer A, Jelsma J, Moyo A. Appreciation of community-based rehabilitation by caregivers of children with a disability. Disabil Rehabil. 1996;18(5):255–60.
-
Nota A, Chikwanha TM, January J, Dangarembizi N. Factors contributing to defaulting scheduled therapy sessions past caregivers of children with built disabilities. Malawi Med J. 2015;27(1):25–8.
-
Devendra A, Makawa A, Kazembe PN, Calles NR, Kuper H. HIV and babyhood disability: a case-controlled report at a paediatric antiretroviral therapy Heart in Lilongwe, Malawi. PLoS One. 2013;eight(12):e84024.
-
Paget A, Mallewa M, Chinguo D, Mahebere-Chirambo C, Gladstone G. "It means you lot are grounded"–caregivers' perspectives on the rehabilitation of children with neurodisability in Malawi. Disabil Rehabil. 2016;38(3):223–34.
-
Alloh D, Nandjui B, Bombo J, Manou B, Twoolys A, Alloukou R, et al. Organizational and operational capabilities of specialist centres for children with psychomotor disability in Abidjan. Ann Phys Rehabil Med. 2009;52(5):414–26.
-
Bayat Thousand. Understanding views of disability in the cote d'Ivoire. Disabil Soc. 2014;29(1):30–43.
-
Yousafzai AK, Edwards K, D'Allesandro C, Lindström 50. HIV/AIDS information and services: the situation experienced by adolescents with disabilities in Rwanda and Uganda. Disabil Rehabil. 2005;27(22):1357–63.
-
Bannink F, Stroeken K, Idro R, Van Hove G. Community knowledge, beliefs, attitudes, and practices towards children with spina bifida and hydrocephalus in Uganda. Int J Disabil Dev Educ. 2015;62(2):182–201.
-
Bunning K, Gona JK, Odera-Mung'ala Five, Newton CR, Geere J-A, Hong CS, et al. Survey of rehabilitation support for children 0–15 years in a rural part of Kenya. Disabil Rehabil. 2014;36(12):1033–41.
-
Magnussen HJA. Childhood disability in rural Zambia: a qualitative study on the utilize of health care services; 2011.
-
Ogunkeyede SA, Adebola And then, Salman A, Lasisi AO. Babyhood hearing loss; a demand for main health care. Int J Pediatr Otorhinolaryngol. 2017;94:117–20.
-
Tekola B, Baheretibeb Y, Roth I, Tilahun D, Fekadu A, Hanlon C, et al. Challenges and opportunities to improve autism services in low-income countries: lessons from a situational analysis in Ethiopia. Global Ment Health. 2016;3:1–11.
-
Okonofua F, Lambo Eastward, Okeibunor J, Agholor K. Advocacy for free maternal and kid health care in Nigeria—results and outcomes. Health Policy. 2011;99(2):131–8.
-
Shillingford L. A step in the right direction. Nursing Standard (through 2013). 2000;xiv(23):52.
-
Aldersey HM, Turnbull Iii HR, Turnbull AP. Intellectual and developmental disabilities in Kinshasa, Democratic Commonwealth of the Congo: causality and implications for resilience and back up. Ment Retard. 2014;52(three):220–33.
-
Akesode FA. Factors affecting the use of primary health intendance clinics for children. J Epidemiol Community Wellness. 1982;36(4):310–iv.
-
Barlindhaug G, Umar E, Wazakili Grand, Emaus Due north. Living with disabled children in Malawi: challenges and rewards. Afr J Disab. 2016;five(1):ane–8.
Acknowledgements
We are grateful to Ms. Paola Durando, Bracken Wellness Sciences Librarian, at Queen's Academy for her support with searching the databases for our scoping review.
Funding
There was no fund for this enquiry written report.
Writer information
Affiliations
Contributions
FN, SS and SG conceptualized and designed the study and conducted the database search; FN and SS analyzed and interpreted the data while SG and MA helped in creating themes and subthemes along with thick description from the reviewed studies. MA and SG prepared the manuscript for periodical submission and responded to the reviewer'south comments. All authors have read and approved the final manuscript for submission.
Corresponding writer
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they accept no competing interests.
Additional data
Publisher's Annotation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1.
A: Reviewed Articles by Selected Country. B: Major Themes of the Findings. C: Barriers to Healthcare Services Access for CwDs. D: Facilitators to Healthcare Services Access for CwDs
Appendix
Appendix
Rights and permissions
Open Access This article is distributed nether the terms of the Creative Eatables Attribution iv.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted employ, distribution, and reproduction in whatever medium, provided you requite appropriate credit to the original author(s) and the source, provide a link to the Creative Eatables license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/goose egg/1.0/) applies to the data made available in this article, unless otherwise stated.
Reprints and Permissions
About this article
Cite this article
Adugna, M.B., Nabbouh, F., Shehata, S. et al. Barriers and facilitators to healthcare admission for children with disabilities in depression and middle income sub-Saharan African countries: a scoping review. BMC Health Serv Res 20, 15 (2020). https://doi.org/x.1186/s12913-019-4822-6
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s12913-019-4822-six
Keywords
- Sub-Saharan Africa
- Barriers
- Children with disabilities
- Wellness services
- Healthcare access
Source: https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-019-4822-6
0 Response to "Impact of Low Income Families Not Accessing Care for Disabled Chidlren"
Post a Comment